Burnout and Cortisol: Why It’s Not Just “High Cortisol”
It’s not always “high cortisol.”
More often, it’s a rhythm that’s been disrupted.
Cortisol is one of the body’s most important hormones, yet it’s often misunderstood. It’s not just your “stress hormone,” it’s deeply involved in how you wake up in the morning, how your energy carries you through the day, how your blood sugar is regulated, how your immune system responds, and how your body prepares for rest at night.
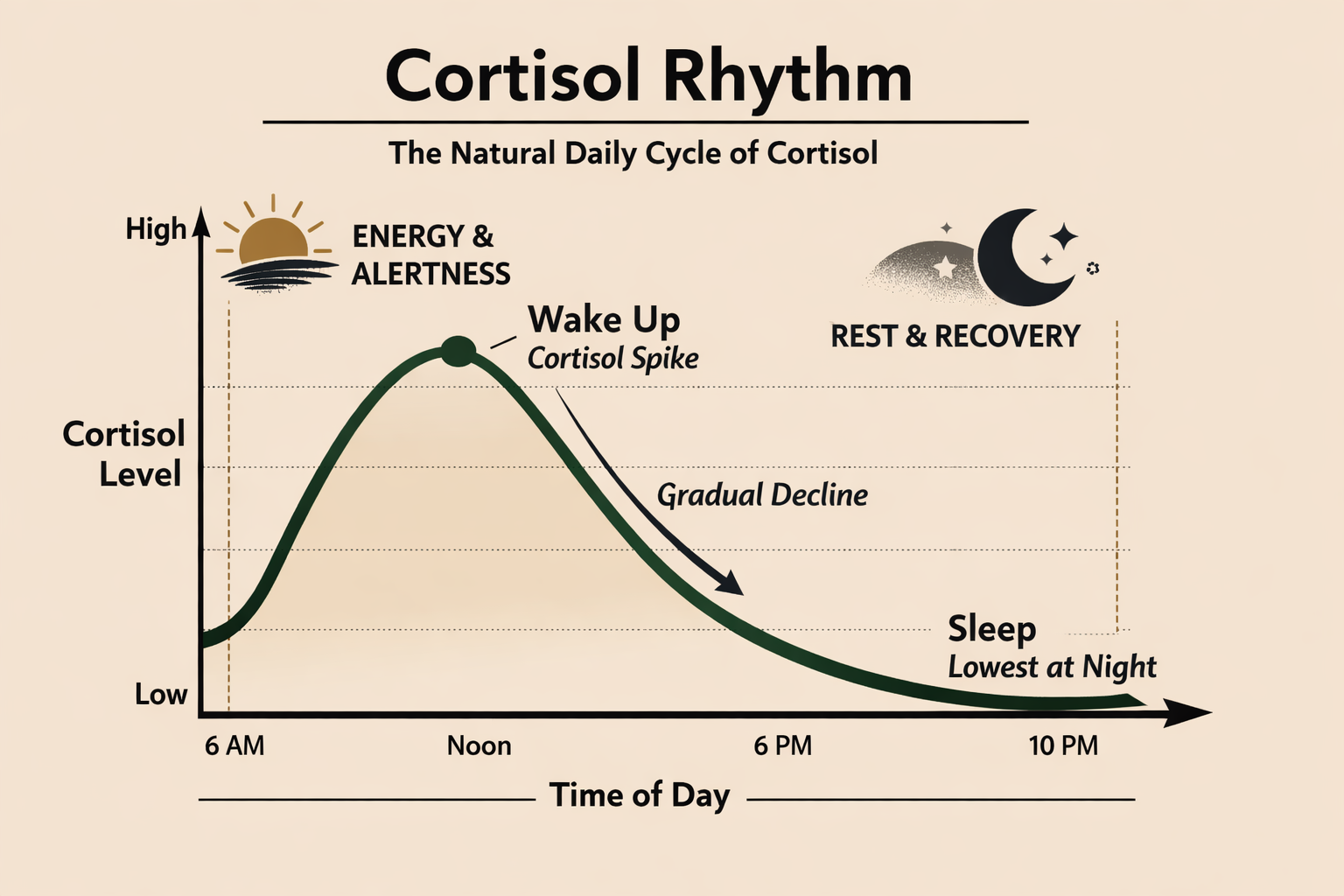
When cortisol is working well, it follows a natural rhythm. It rises in the morning to help you feel alert, focused, and ready to start your day, then gradually declines as the day goes on, allowing your body to shift into a more relaxed state in the evening and eventually fall asleep.
Your cortisol should peak in the morning to energize you, then gradually decline so your body can rest at night.
When it doesn’t, you begin to feel off.
When that rhythm becomes disrupted, the body starts to feel it.
You might notice that mornings feel heavy and slow, like it takes everything just to get going. Or the opposite, feeling wired, anxious, and overstimulated. Energy may dip in the afternoon, only to pick back up again at night, leaving you tired but unable to fully rest. Sleep becomes lighter, more fragmented. You might get sick more often, feel more reactive to stress, or notice changes in weight, mood, or digestion that don’t quite make sense.
This is where the conversation around cortisol often gets simplified into “it’s too high,” but that’s rarely the full picture. Cortisol is constantly fluctuating throughout the day, and what matters most is not just how much of it you have, but when it’s being released and how your body is responding to it.
In practice, what I see more often is dysregulation. Cortisol that’s too low in the morning, making it difficult to wake and feel energized. Cortisol that stays elevated into the evening, making it hard to wind down. Or a flattened pattern altogether, where the body no longer has the same capacity to respond to stress in a dynamic way. This is often where burnout begins to show up.
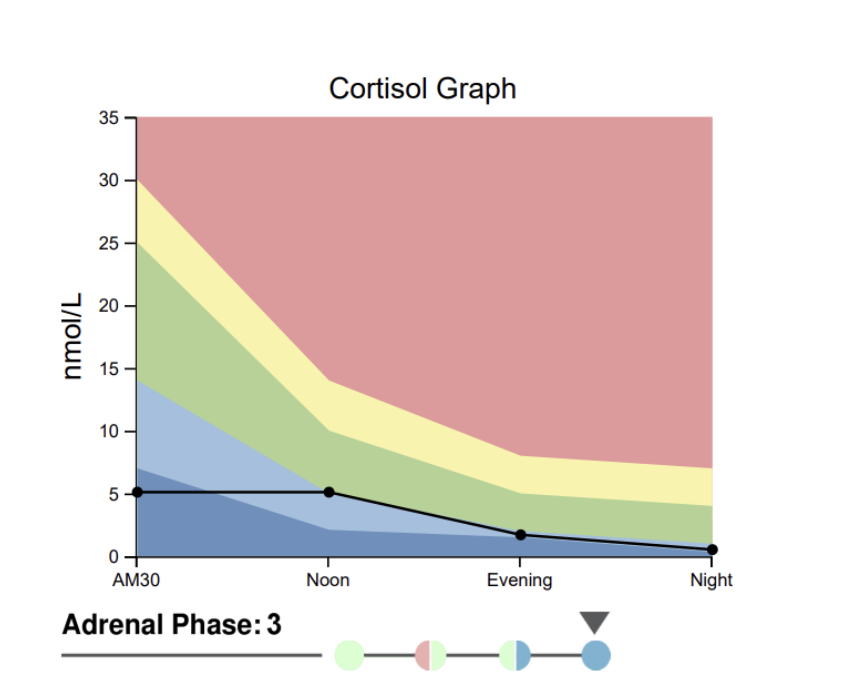
This patient originally came in concerned about “high cortisol,” but testing revealed a flattened, dysregulated pattern before treatment.
In burnout states, cortisol often becomes blunted and poorly timed.
The body doesn’t move from “stressed” to “burnt out” overnight. There is usually a progression. Initially, cortisol may be elevated, leaving you feeling alert but on edge. Over time, the system begins to adapt, and other hormones like DHEA start to decline, impacting energy, focus, and resilience. If this continues, the system can become depleted, and cortisol output may drop, leaving you feeling exhausted, less resilient, and slower to recover.
This is why the idea of simply “lowering cortisol” can be misleading. Cortisol is essential. You need it to get out of bed, to regulate blood sugar, to support immune function, and to respond to life’s demands. The goal is not to suppress it, but to bring it back into a rhythm that feels supportive to your body.
It’s also important to recognize that cortisol does not operate in isolation. It’s influenced by your nervous system, your sleep, your gut health, your hormone balance, and your overall stress load. This is why a one-size-fits-all approach rarely works, and why the same symptom can come from very different patterns. Because of this, simply reaching for a “cortisol” supplement isn’t always the most supportive first step. Some herbs can feel a bit too activating for a system that’s already sensitive or depleted, and the way something is timed or combined can make a meaningful difference in how the body responds. Often, the goal is to understand what your body is asking for, and to support it in a way that feels gentle, aligned, and sustainable.
Because cortisol is constantly changing throughout the day, testing needs to reflect that. A single blood test offers only a snapshot, whereas saliva testing allows us to see how cortisol rises and falls across the day. More comprehensive testing, such as the DUTCH hormone test, can provide even deeper insight into cortisol patterns, DHEA levels, and how your body is processing stress on a hormonal level. This gives us a much clearer understanding of where support is needed and how to approach it in a way that’s individualized and sustainable.
In practice, the focus is on regulation, not suppression. Supporting the nervous system, stabilizing blood sugar, improving sleep quality, and addressing underlying contributors such as gut health or inflammation all play a role. Acupuncture, targeted nutrition, lifestyle adjustments, and when appropriate, supplementation, can help guide the body back into a more balanced state.
If you’ve been feeling off, tired, wired, reactive, or like your body isn’t responding the way it used to, there is usually a reason. These patterns are not random.
They’re the body’s way of communicating.
If you’re curious about whether cortisol may be playing a role in how you’re feeling, I offer complimentary 15-minute consultations to talk through what’s been coming up for you and explore whether this approach feels like the right next step.
If you choose to move forward, it would be an honour to be trusted with your health journey.